Grapevine, TX – March 14, 2025 Mind Above Matter Partners with Maples Treatment Center and Meridell Achievement Center to Host Affirmation Box Workshop at House Shine
In celebration of St. Patrick’s Day 2025, participants from Maples Treatment Center and Meridell Achievement Center joined Mind Above Matter in a creative and therapeutic workshop. The focus of the event was to design and create personalized affirmation boxes. These boxes serve as a repository for positive affirmations, encouraging individuals to start their day with a positive mindset.
Participants had the option to write their own powerful daily affirmations or select from a shared pool, adding an element of surprise and community support. The event incorporated the symbolic shamrock, representing luck and positivity, to further enhance the uplifting experience.


The Maples Treatment Center focuses on helping teenage girls struggling with their mental health, including trauma, disordered eating, and/or substance use. They provide a safe place for residents and their families to work together on their unhealthy past decisions. The Maples uses respect, accountability, and self-love to encourage healthier choices.
Their residential program is staffed with trained mental health professionals that provide evidence-based therapies. They offer activities that support structure and accountability while having an environment that promotes creativity, mindfulness, goal setting, and self-care.

The Meridell Achievement Center in Liberty Hill, Texas, is a residential treatment center specializing in behavioral and neurobehavioral programs for adolescents aged 10-17. The center has provided specialized care for children and adolescents for over 60 years.
Meridell treats adolescents with a variety of diagnoses including bipolar disorder, ADHD, PTSD and high-end autism spectrum disorders, among others. Meridell Achievement Center is accredited by the Joint Commission and licensed by the state of Texas. The center also supports the whole family.
Mind Above Matter was honored to collaborate with Maples Treatment Center and Meridell Achievement Center, both renowned for their commitment to mental wellness. These partnerships underscore our shared dedication to providing valuable mental health resources and support to our communities.
The practice of using daily affirmations has been shown to have numerous benefits of affirmations and benefits of positive affirmations. Scientific research supports the notion that regularly affirming positive statements can rewire the brain, reducing stress and increasing feelings of self-worth. Studies indicate that affirmations can activate areas of the brain associated with self-related processing and reward, leading to improved mental and emotional well-being. The scientific benefits of affirmations include:
By creating affirmation boxes, participants are equipped with a practical tool to integrate these benefits into their daily lives.
“We are thrilled to have partnered with Maples Treatment Center and Meridell Achievement Center for this meaningful event,“ said Jesse Cordova, Director of Business Operations at Mind Above Matter. “Creating affirmation boxes is a wonderful way to instill positivity and encourage self-reflection. We are committed to providing resources that support mental wellness and look forward to continuing our work in the community.”
At Mind Above Matter, we believe that everyone deserves access to quality mental health care. If you or a loved one are seeking mental health services, we encourage you to reach out to our team of qualified mental health professionals. We offer a range of services tailored to meet individual needs. To learn more about our offerings and access valuable mental health resources, visit our website today. Our team is here to support you on your journey to mental wellness.
For daily affirmations and mental health tips, follow Mind Above Matter on Instagram, Facebook, and LinkedIn.
We proudly serve Keller and Burleson, Texas as well as multiple Texas school districts including Carrollton Farmers Branch, Irving, and Waxahachie ISDs.
Related Posts: 2025 Resiliency & Recovery Conference of Fort Worth
Spring has sprung, and with it comes a sense of renewal and possibility. Spring’s arrival brings a chance for renewal, and that extends to your mental well-being. This season offers unique opportunities to engage in refreshing mental health activities.
Let’s explore how you can leverage the energy of spring to engage in rejuvenating mental health activities.
Spring’s arrival often brings a natural lift in mood. The increased sunlight triggers the production of vitamin D, a crucial nutrient for mental health. However, this season can also present challenges. Some individuals experience “reverse SAD,” feeling overwhelmed by the surge of social activities and expectations. It’s essential to proactively manage your mental health during this transitional period.
Increased sunlight exposure leads to higher vitamin D production in the body. Vitamin D plays a crucial role in regulating mood by influencing serotonin levels, a neurotransmitter associated with happiness and well-being.
Spending time in nature has been shown to reduce levels of cortisol, the stress hormone. Studies have demonstrated that exposure to natural environments can promote relaxation, improve mood, and enhance cognitive function.

Embrace the outdoors and let nature be your therapist. Engaging in outdoor spring mental wellness activities can significantly enhance your well-being.
Grounding and Connection
Immerse yourself in nature by taking a walk or hike. Feel the earth beneath your feet and reconnect with the natural world.
Mindful Walking Tips
Practice mindful walking by focusing on your senses and breathing deeply. Notice the textures of the path, the sounds of birdsong, and the scents of blooming flowers.
Therapeutic Nurturing
Engage in the therapeutic act of gardening or planting. Nurturing plants can be a rewarding experience that fosters a sense of accomplishment and reduces stress.
Creating a Small Garden
Even a small space can become a sanctuary. Create a small indoor or outdoor garden to bring the beauty of nature into your home.
Mood-Boosting Movement
Physical activity is a powerful mood booster. Engaging in outdoor exercise can release endorphins, natural chemicals that have mood-elevating effects.
Spring Activities
Enjoy activities like cycling, jogging, or outdoor yoga. Take advantage of the warmer weather and spend time in nature while getting some exercise.
Setting Realistic Goals
Start small and gradually increase your activity level. Set realistic fitness goals and celebrate your progress along the way.
Sensory Awareness
Practice mindful observation by simply sitting outside and observing nature. Pay attention to the sights, sounds, and smells around you.
Focused Attention
Engage in focused attention by observing a single object or phenomenon in nature, such as a bird, a flower, or a cloud.

Even when indoors, you can cultivate a sense of calm and well-being.
Decluttering and Organizing
Engage in a spring cleaning of your physical and mental space. Decluttering and organizing your living environment can create a sense of calm and reduce stress.
Reducing Stress
A tidy and organized space can promote mental health spring clarity and reduce feelings of overwhelm.
Art Therapy
Engage in creative activities like painting, drawing, or sculpting. Art therapy can be a powerful tool for processing emotions and promoting self-expression.
Writing and Music
Explore writing, journaling, or playing music. These activities can provide a healthy outlet for emotions and promote relaxation.
Processing Emotions
Creative outlets can help you process emotions, gain insights into your thoughts and feelings, and develop a deeper understanding of yourself.
Guided Meditation
Use apps or online resources to guide you through meditation exercises.
Simple Breathing Exercises
Practice simple breathing exercises, such as deep breathing or diaphragmatic breathing, to calm your mind and reduce stress.
Reducing Anxiety
Regular mindfulness and meditation practices can help reduce anxiety, improve focus, and promote overall well-being.
Scheduling Social Time
Make a conscious effort to schedule time for social interaction with friends and family.
Interactive Activities
Plan interactive activities, such as game nights, potlucks, or outdoor picnics, to foster social connection and enjoyment.
Combating Isolation
Social connection is vital for spring and mental health. Make an effort to combat social isolation by engaging in activities that bring you together with others.
Reflect on Growth and Change
Use journaling prompts to reflect on personal growth and change. Consider questions like: “What new things are you looking forward to this spring?” or “How can you grow and change this season?”
Embrace the Feeling of Renewal
Explore the feeling of renewal associated with spring. Write about what renewal means to you and how you can cultivate a sense of renewal in your own life.
Spring offers a unique opportunity to prioritize your mental health. By engaging in these mental health activities, you can cultivate a sense of well-being and resilience. At Mind Above Matter, we’re committed to supporting your mental health journey. Whether you’re seeking individual therapy, family counseling, or educational resources, we’re here to help. Contact our offices or visit our website to learn more about our mental health services and how we can support you this spring and beyond.
1. What are mental health activities?
Mental health activities are intentional practices that help improve emotional well‑being, reduce stress, and support psychological balance through self‑care and coping strategies.
2. How often should I do mental health activities?
Regularly engaging in mental health activities daily or several times a week is most effective for managing stress and maintaining emotional resilience.
3. Can simple activities really improve my mental health?
Yes. Simple practices like journaling, mindful breathing, or a nature walk can reduce anxiety, enhance mood, and support overall wellness.
4. Are group activities helpful for mental well‑being?
Group activities can boost emotional health by building social connection, improving self‑esteem, and offering peer support.
5. Do mental health activities help with stress and anxiety?
Absolutely. Activities designed for mental health can lower stress, manage anxiety, and support coping skills when practiced consistently.
Related: Summer Mental Health Tips for the Warmer Months
Music is a universal language that transcends cultural boundaries and speaks directly to the soul. From ancient rituals to modern playlists, it has been an integral part of the human experience. But its power extends far beyond entertainment. Music possesses a remarkable ability to influence our emotions, thoughts, and physical well-being, making it a valuable therapeutic tool in mental health.
This article explores the connection between music therapy and mental health, exploring its definition, history, neurological effects, and diverse benefits for individuals seeking mental wellness.
Music therapy is a recognized healthcare profession that utilizes music interventions to address individualized goals within a therapeutic relationship. It’s more than just playing music; it’s a structured, evidence-based practice delivered by credentialed professionals. Music therapists are highly trained to assess each individual’s unique needs and design interventions that may encompass a variety of musical experiences. These can include creating music through songwriting or improvisation, singing familiar tunes, moving to music, actively listening to specific pieces, and engaging in discussions about the emotional responses evoked by music.
The cornerstone of effective music therapy is the therapeutic relationship between the client and the therapist. This relationship provides a safe, supportive, and non-judgmental space for individuals to explore their inner world, express their emotions, develop coping mechanisms, and ultimately improve their overall well-being. Music therapists possess a deep understanding of the psychological, emotional, cognitive, and social impact of music. They leverage this knowledge to guide clients through musical experiences that promote healing and growth.
The use of music for healing dates back to ancient civilizations, but music therapy as a formal profession emerged in the 20th century. Its development was significantly influenced by the profound experiences of musicians who volunteered in hospitals during World Wars I and II. These musicians witnessed firsthand the positive effects of music on patients’ emotional and physical states, observing how it could alleviate pain, reduce anxiety, and foster a sense of connection during times of great hardship.
Fueled by these observations, formal training programs in music therapy began to take shape, and the profession gradually gained recognition within the broader healthcare field. Over the ensuing decades, rigorous research has continued to expand our understanding of the therapeutic benefits of music. This growing body of evidence has led to the increasing integration of music therapy into a wide array of treatment settings, including mental health facilities, general hospitals, rehabilitation centers, schools, community centers, and private practices.
The human brain exhibits a complex and fascinating response to music. Advanced neuroimaging studies have revealed that listening to or creating music activates a multitude of brain regions simultaneously. These regions are intricately involved in processing emotions, cognition, sensory information, and motor control. This widespread and integrated brain activity is believed to play a crucial role in the therapeutic effects of music.
Music has the power to influence the release of various neurotransmitters, which are chemical messengers in the brain. For example, it can stimulate the release of dopamine, a neurotransmitter associated with pleasure, motivation, and reward. This can explain why music can be effective in elevating mood and fostering a sense of well-being. Conversely, music can also help regulate the release of cortisol, a hormone associated with stress. This can contribute to its ability to reduce anxiety and promote relaxation. Furthermore, music has been shown to enhance neural plasticity, the brain’s remarkable ability to reorganize itself by forming new neural connections. This is a critical process for learning, memory, and recovery from neurological conditions.
Music therapy offers a diverse range of benefits for individuals seeking to improve their mental health. One of its most powerful attributes is its capacity to provide a non-verbal outlet for emotional expression. This can be particularly valuable for individuals who struggle to articulate their feelings verbally, such as those who have experienced trauma, have communication difficulties, or are navigating complex emotions. Music can offer a safe and creative way to communicate and process these emotions.
Beyond emotional expression, music is a potent tool for stress reduction. Listening to calming music can elicit physiological changes, such as slowing down the heart rate, lowering blood pressure, and reducing muscle tension. Music therapy interventions can equip individuals with relaxation techniques and coping skills that they can use to manage stress and anxiety in their daily lives. In addition, music therapy can enhance self-esteem and confidence, improve social skills and interaction, and foster a sense of connection and belonging, particularly in group therapy settings.

Depression can significantly impair mood, motivation, and overall quality of life. Music therapy provides a supportive and engaging avenue for individuals to explore and process the complex emotions associated with depression, such as sadness, hopelessness, and anger. Interventions may include songwriting, lyric analysis, listening to emotionally resonant music, and playing instruments. These activities can help individuals express their feelings in a healthy way, increase motivation, promote social interaction, and cultivate a sense of hope and empowerment.
Attention-deficit/hyperactivity disorder (ADHD) is characterized by challenges with attention, impulsivity, and hyperactivity. Music therapy can offer structured and engaging strategies to improve focus, self-regulation, and cognitive function in individuals with ADHD. Interventions may incorporate structured drumming activities to enhance attention span, movement and music to release excess energy and improve coordination, and songwriting to express emotions and develop communication skills. The rhythmic and predictable nature of music can provide a sense of organization and structure, which can be particularly beneficial.
Autism spectrum disorder (ASD) can affect communication, social interaction, and sensory processing. Music therapy offers a unique and effective way for individuals with ASD to enhance communication, social skills, and emotional expression. Interventions may involve singing, playing instruments, improvising music, and using music to facilitate social interaction and connection. Music can provide a predictable and engaging medium for communication, allowing individuals with ASD to connect with others and express themselves in novel and meaningful ways. Music therapy can also aid in sensory integration and reduce anxiety.
The versatility of music therapy extends to a wide range of other mental and physical health conditions. For individuals with Parkinson’s disease, music therapy can be used to improve motor skills, gait, and speech. The rhythmic cues inherent in music can help regulate movement and enhance coordination. In Alzheimer’s care, music therapy can be a powerful tool to evoke memories, reduce agitation, and improve mood in individuals with dementia. Familiar songs can tap into preserved cognitive functions and provide a sense of comfort and connection. Music therapy is also utilized in pain management, rehabilitation programs, and end-of-life care.

Music therapy encompasses a variety of approaches and techniques, each tailored to the specific needs of the individual or group.
At Mind Above Matter, we recognize the profound therapeutic value of creative expression. In addition to our other mental health services, we offer weekly music and art therapy programs at our clinics in Keller and Burleson, Texas. These programs provide a unique and engaging way for individuals to explore their feelings, develop coping skills, and enhance their overall quality of life. Our music therapy offerings include group therapy sessions, providing a supportive and collaborative environment for individuals to connect with others and express themselves through music. We also provide specialized children’s music therapy programs, tailored to the developmental needs and challenges of adolescents as young as 9. All of our music and art therapy programs are facilitated by licensed professionals holding a music therapy license, ensuring a high standard of care and clinical expertise.
Music therapy offers a powerful and effective approach to promoting mental wellness. From its capacity to facilitate emotional expression to its positive impact on brain function, music has a significant role to play in supporting individuals on their journey to healing and growth. For more detailed information on music therapy, please visit the American Music Therapy Association website.
If you or someone you know could benefit from music therapy or other mental health services, we encourage you to reach out. Our team at Mind Above Matter is here to provide compassionate and effective care. Contact us today to learn more about our programs and how we can support your journey to well-being.
How does music therapy help mental health?
Music therapy supports mental health by reducing stress, improving mood, enhancing emotional expression, and promoting relaxation. It can also help regulate brain chemicals like dopamine and cortisol, which influence mood and stress levels.
Can music therapy help with anxiety and depression?
Yes, music therapy is commonly used to treat anxiety and depression. It provides a safe outlet for emotional expression, helps regulate mood, and can increase motivation and social connection through structured activities.
Is music therapy backed by science?
Yes, research shows that music activates multiple areas of the brain and can positively affect neurotransmitters, stress hormones, and neural pathways. These neurological effects support its use as a therapeutic tool in mental health treatment.
What happens during a music therapy session?
A session may include listening to music, discussing emotional responses, writing songs, playing instruments, or guided relaxation exercises. The structure depends on the individual’s goals and needs.
Who can benefit from music therapy?
Music therapy can benefit people of all ages, including those with depression, anxiety, ADHD, autism, trauma, neurological conditions, and even individuals seeking general emotional wellness.
Related Links: Creating Connections: The Benefits of Group Therapy
The impact of trauma is a deeply personal and multifaceted experience. Recognizing the diverse ways in which individuals are affected, the mental health field has established a comprehensive framework known as the five levels of trauma care.
This tiered system ensures that individuals receive support tailored to the intensity of their experiences and their unique needs, guiding them on a path toward healing and recovery. Understanding these levels can provide clarity for those seeking help and empower professionals to deliver the most effective and compassionate care.
A tiered approach to trauma care acknowledges that not all traumatic experiences have the same impact, and individuals will require varying levels of support. This system prevents a one-size-fits-all approach, which can be ineffective or even re-traumatizing.
By matching the intensity of the intervention with the individual’s level of distress and the complexity of their trauma history, this framework optimizes the healing process. It emphasizes a continuum of care, allowing individuals to access the right support at the right time, progressing through levels as needed.
The initial level of trauma care focuses on providing individuals with fundamental knowledge about trauma and its common effects. This stage empowers individuals to understand their reactions and utilize self-help strategies to manage their well-being. Often suitable for those who have experienced potentially traumatic events but aren’t currently facing significant distress or impairment, Level 1 aims to build resilience and normalize the recovery process.
Psychoeducation at this level involves offering accessible information about the body’s stress response, typical trauma symptoms like sleep disturbances and anxiety, and the general trajectory of healing. Resources such as informative websites, self-help books, and introductory workshops can provide a broad understanding of trauma’s impact.
Self-help strategies are a cornerstone of Level 1 care. These often include teaching basic stress management techniques such as relaxation exercises and mindfulness practices. Developing healthy lifestyle habits – regular exercise, balanced nutrition, and sufficient sleep – are also emphasized as they significantly contribute to overall mental and emotional resilience.
Moving beyond foundational knowledge, Level 2 trauma care offers more direct support through brief interventions and early support systems. This level is designed for individuals experiencing mild to moderate distress or functional challenges in the aftermath of a traumatic event. Brief therapy models, crisis counseling, and peer support groups facilitated by trained professionals are common interventions.
Brief therapy approaches at this stage are typically time-limited and focus on addressing specific symptoms or developing immediate coping skills. Crisis counseling offers immediate support during or shortly after a traumatic event, helping individuals regain a sense of safety and emotional equilibrium.
Support groups provide a vital space for individuals with shared experiences to connect, offer mutual understanding, and learn from one another. This sense of community can be incredibly validating and help normalize trauma responses in the early stages of recovery.
Level 3 trauma care involves more intensive and sustained outpatient therapy for individuals who have developed trauma-related disorders, such as PTSD, Acute Stress Disorder, or those grappling with the effects of childhood trauma therapy. This level utilizes evidence-based psychotherapies specifically tailored to address the complex psychological and emotional sequelae of trauma. The primary goals include processing traumatic memories, reducing intrusive symptoms, addressing avoidance behaviors, and enhancing emotional regulation skills.
Common therapeutic modalities employed at this level include cognitive behavioral trauma therapy (CBT-T), Eye Movement Desensitization and Reprocessing (EMDR), and other trauma-informed approaches. These therapies guide individuals through the careful and gradual processing of traumatic experiences within a safe and supportive therapeutic relationship.
Therapists at this level are skilled in helping individuals manage intense emotions, develop effective coping mechanisms for trauma triggers, and challenge negative, trauma-related thought patterns. The overarching aim is to facilitate deep healing, reduce the severity of symptoms, and improve overall daily functioning and quality of life for those impacted by trauma.
Level 4 trauma care offers more intensive and structured treatment through Intensive Outpatient Programs (IOPs) and Partial Hospitalization Programs (PHPs). These programs provide several hours of therapy multiple days a week, offering a significantly higher level of support and structure compared to traditional weekly outpatient therapy. This level is often beneficial for individuals experiencing substantial functional impairment, high levels of distress, or those requiring more intensive stabilization and skill-building. This can be particularly helpful for individuals requiring attachment trauma treatment or navigating the complexities of complex trauma treatment.
IOPs and PHPs for trauma integrate various therapeutic modalities, including individual therapy, group therapy, psychoeducation, and skills training focused on emotional regulation and coping strategies. Multidisciplinary teams, comprising therapists, psychiatrists (for medication management when necessary), and other mental health professionals, collaborate to create and implement personalized treatment plans. This intensive level of care provides a supportive and structured environment crucial for addressing significant trauma-related challenges and fostering stabilization.
The most intensive level of trauma care, Level 5, involves treatment within inpatient or residential settings. This level is reserved for individuals experiencing severe trauma-related symptoms that pose a significant risk to their safety or severely impair their ability to function in daily life. This may include those in acute crisis, at high risk of self-harm or harming others, experiencing severe dissociation, or managing complex co-occurring mental health and substance use disorders. The primary focus is on providing a secure and contained environment for immediate stabilization, intensive therapeutic intervention, and comprehensive crisis management.
Inpatient and residential trauma programs offer continuous 24/7 support and supervision, alongside intensive individual and group therapy, psychiatric care, and medical management. The goal is to stabilize acute symptoms, ensure the safety of the individual, and initiate the process of addressing the underlying trauma within a highly structured and supportive setting. The duration of stay in these programs is tailored to the individual’s unique needs and progress. Following this intensive phase, individuals typically transition to a lower level of care to continue their journey of recovery.
Navigating the complexities of trauma requires a nuanced and individualized approach. Understanding the five levels of trauma care provides a roadmap for both individuals seeking support and professionals dedicated to facilitating healing. Recognizing the different levels ensures that individuals receive the appropriate intensity of care, fostering resilience and promoting lasting recovery.
If you or someone you know is seeking support on their journey to healing from trauma, Mind Above Matter offers a range of outpatient therapy services at our locations in Keller and Burleson, Texas. We also provide virtual therapy services throughout Texas. We are committed to providing accessible and compassionate care to support your mental well-being.
Related: What are the 5 Levels of Trauma Care?
MIND ABOVE MATTER SPONSORS DENTON NEIGHBORS NETWORK EVENT
Denton, TX – May 28, 2025 – Mind Above Matter, a leading provider of comprehensive mental health services in Texas, proudly sponsored the Denton Neighbors Network monthly mental health networking event yesterday, May 28, 2025. Held at Patchouli Joe’s Bookstore, the gathering brought together a diverse group of mental health professionals dedicated to strengthening community-based care.
The event, hosted monthly by Neighbors Counseling in Denton, serves as a vital platform for creating a robust network of mental health providers. Its core purpose is to facilitate client referrals, encourage discussions on best practices and new treatment methods, and foster the sharing of essential resources. As this month’s sponsor, Mind Above Matter was given the opportunity to highlight its extensive services, including its outpatient programs in Keller and Burleson, and its innovative iMatter school-based mental health program.
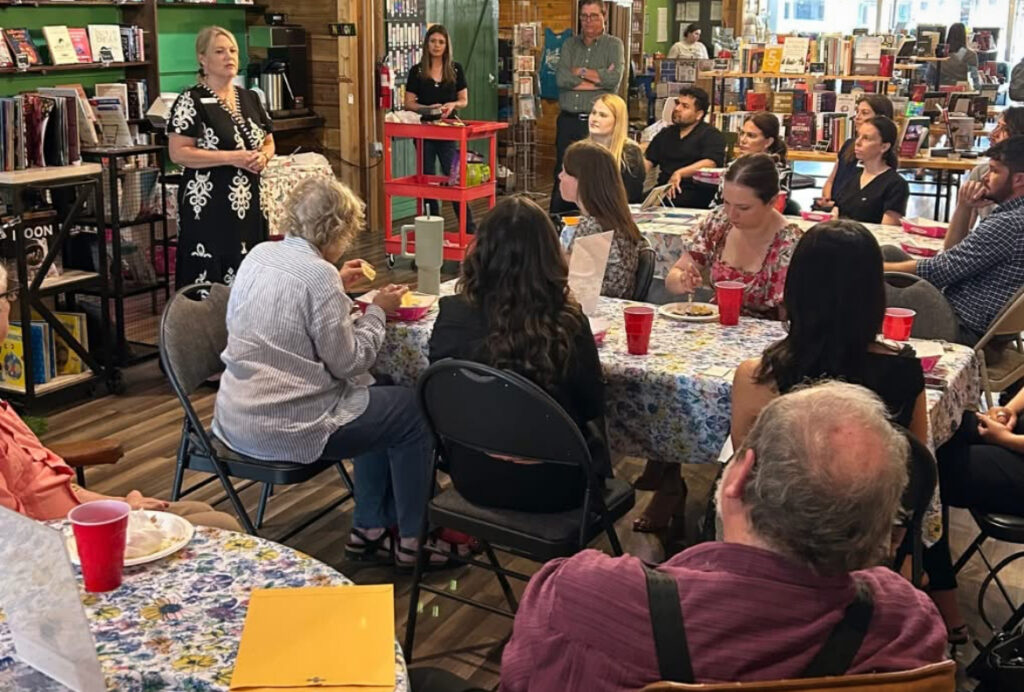
Attendees included a wide array of professionals, such as therapists, business development representatives, school advocates, and representatives from organizations like NAMI. The collaborative atmosphere underscored the collective commitment within the mental health community to enhance access to care and ensure individuals receive the most appropriate treatment. By fostering these relationships, Mind Above Matter continues its mission to close the gap in mental health care and treatment across Texas.

“We were thrilled to sponsor the Denton Neighbors Network event and engage with so many passionate professionals committed to mental wellness,” said Tracie Owen, Community Relationships Representative. “These collaborative efforts are essential for building stronger referral pathways and ensuring that individuals and families in our communities receive the comprehensive support they need, whether through our clinic-based services or our school programs.”
About Mind Above Matter: Mind Above Matter is a dedicated mental health organization providing comprehensive outpatient therapy services for adolescents and adults across Texas, with brick-and-mortar locations in Keller and Burleson. Offering Partial Hospitalization Programs (PHP), Intensive Outpatient Programs (IOP), individual therapy, medication management, and specialized programs like the iMatter school-based mental health initiative, Mind Above Matter is committed to delivering accessible, high-quality, and compassionate care to promote lasting well-being.
Related: 2025 St. Patty’s Day Affirmation Box Workshop
The last bell rings, textbooks are shelved, and the doors swing open to a season of sunshine and freedom. For many students, summer break is synonymous with fun and relaxation. However, beyond the obvious joys of vacations and late mornings, this extended pause in the academic year plays a profoundly critical role in fostering positive mental health. In an era where academic pressures are escalating, understanding why summer break is good for students’ mental health is more important than ever.
Today’s students navigate a high-pressure environment, juggling demanding curricula, the intensity of standardized testing, a packed schedule of extracurricular activities, and complex social dynamics. This constant state of high-alert performance can lead to significant stress, anxiety, and even burnout, impacting not just academic performance but overall mental well-being. The relentless pace leaves little room for minds to genuinely unwind and recharge.
Summer break, therefore, emerges as a vital period for mental health rejuvenation. It’s a necessary pause in the academic cycle that allows students to disconnect from stressors, reconnect with themselves, and engage in activities that foster well-being. Today, we will explore the key benefits of summer break, highlighting how these contribute to a healthier, more balanced mental state for students.
The structured and often demanding environment of school can lead to chronic stress in students. From the cognitive load of constantly learning new material to the pressure of deadlines and the intricate social dynamics of school life, a student’s brain is under constant mental exertion. Summer break offers a crucial respite, allowing the mind to decompress from this continuous intellectual and emotional demands. This period of reduced demands helps to lower cortisol levels, the body’s primary stress hormone, and effectively resets the body’s stress response system.
This reduction in stress directly contributes to preventing burnout, a state that can manifest in students as emotional exhaustion, a cynical attitude towards school, and a diminished sense of personal accomplishment. When students are burnt out, their motivation wanes, and their capacity to engage with learning or social activities decreases significantly. Summer provides the essential time needed for students to genuinely recharge their mental batteries, regaining their natural curiosity, enthusiasm, and motivation for the upcoming academic year. It’s not just a break; it’s a profound opportunity for their minds to rest and recover.
In modern childhood and adolescence, the role of unstructured play has unfortunately diminished, often supplanted by highly organized activities, scheduled lessons, and extensive screen time. Summer break naturally opens up invaluable opportunities for free play, where students can explore their interests without external rules, performance expectations, or the pressure to achieve a specific outcome. This type of play, characterized by self-direction and intrinsic motivation, is vital for developing crucial skills such as problem-solving, emotional regulation, and social competencies outside of a structured environment.
Moreover, this period of unstructured time actively nurtures creativity. When students are not bound by rigid curriculum guidelines or specific assignments, their minds are free to wander, experiment, and imagine. This freedom allows them to delve deeper into personal hobbies, read for pure pleasure, or simply engage in imaginative thinking without constraints. Such activities are crucial for fostering cognitive development, emotional expression, and a healthy sense of self. Summer truly provides a fertile ground for self-discovery and innovation that is often curtailed during the school year.
The demanding schedules of school often lead to widespread chronic sleep deprivation among students. Early start times, coupled with hours dedicated to homework, participation in numerous extracurricular activities, and the pervasive presence of social media, frequently result in insufficient and irregular sleep patterns. This chronic lack of quality sleep significantly impairs a student’s cognitive function, hinders their ability to regulate emotions, and diminishes their overall mental resilience, making them more susceptible to stress and anxiety.
Summer break provides the ideal opportunity to reset these disrupted sleep patterns. With fewer fixed obligations like early alarms or late-night study sessions, students can naturally adjust to a more aligned circadian rhythm, allowing them to achieve the adequate and restorative rest that their developing brains and bodies desperately need. Improved sleep directly translates to a more positive mood, reduced irritability, enhanced concentration, and a stronger, more effective ability to cope with stressors when they return to school. This natural recalibration of sleep cycles is a cornerstone of mental well-being.
While school life inherently offers continuous social interaction, it can also paradoxically be a significant source of social pressure, constant peer comparison, and even bullying, which can negatively impact a student’s self-esteem and mental health. Summer break provides a welcome opportunity for students to broaden their social horizons beyond the immediate school environment. They can connect with friends from different social circles, forge new bonds in less competitive settings, or simply spend more quality, relaxed time with family members without the underlying tension of academic schedules. This diversification of social interactions can significantly reduce social anxiety and pressure often associated with school dynamics.
Furthermore, the increased free time during summer facilitates deeper engagement with family members through shared activities, travel, or simply more spontaneous interactions. It also opens doors for participation in community events, volunteering, or enrolling in summer camps, fostering new friendships and a stronger sense of belonging outside of academic settings. These varied and often lower-pressure social interactions are crucial for healthy social-emotional development, teaching students different forms of communication and connection that contribute to their overall mental well-being.
The typical school day often necessitates prolonged periods of sitting in classrooms, leading to a largely sedentary lifestyle for many students. This pervasive lack of consistent physical activity can profoundly impact mental health, contributing to feelings of sluggishness, a diminished mood, and decreased energy levels, which can exacerbate existing emotional challenges.
Summer break naturally encourages more outdoor time and increased physical activity. Whether it’s through organized sports, swimming, hiking, cycling, or simply spending leisurely time in nature, increased movement and exposure to natural environments are proven mood boosters. Direct sunlight exposure contributes to the body’s production of Vitamin D, which plays a role in mood regulation, and helps regulate serotonin levels in the brain. Moreover, physical activity is a powerful stress reliever and a natural antidepressant. Connecting with nature fosters a profound sense of calm, reduces rumination, and enhances overall well-being, further solidifying the link between physical and mental health.
In conclusion, summer break serves as far more than just a simple vacation from school. It is a critical period that offers a holistic rejuvenation for students’ mental health. By providing essential opportunities for stress reduction, fostering unstructured play and creativity, improving sleep patterns, enhancing social connections beyond school, and promoting crucial physical activity and engagement with nature, summer break plays an indispensable role in a student’s overall well-being. This period of essential reset and growth allows young minds to decompress, rebuild resilience, and develop crucial coping mechanisms.
Ultimately, students who fully embrace these myriad benefits are far more likely to return to school feeling refreshed, resilient, and better equipped to handle the academic and social challenges of the coming year. At Mind Above Matter, we understand the profound impact of mental health on every aspect of a student’s life. We are proud to offer comprehensive mental health services in Keller and Burleson, Texas. We also deeply value our partnerships with Frisco ISD, Irving ISD, and Waxahachie ISD to provide essential student mental health services even during summer break, ensuring continuous support. If you or a student in your life needs mental health support, please visit our dedicated iMatter service page for more information.
Related Links: Refreshing Spring Mental Health Activities
Life can present challenges that shake us to our core. For some, experiencing or witnessing a terrifying event can lead to the development of Post-Traumatic Stress Disorder (PTSD). This is a complex mental health condition that extends far beyond a typical stress response; it involves a persistent and often debilitating set of symptoms that can significantly impact daily life. PTSD is characterized by symptoms falling into distinct categories, often far more numerous and varied than generally recognized. Understanding the full scope of these symptoms is crucial for accurate diagnosis and effective PTSD treatment.
Identifying the specific 17 symptoms of PTSD is vital for both those who may be suffering and their loved ones, as well as for mental health professionals. Gaining a comprehensive understanding of the full spectrum of the 17 symptoms (as recognized in various diagnostic criteria, such as the DSM-5) can lead to earlier recognition, more precise diagnosis, and ultimately, more effective interventions. This knowledge also plays a significant role in destigmatizing the condition by framing it as a recognizable and treatable set of responses to trauma, rather than a personal failing or weakness.

Intrusion symptoms are often considered the hallmark of PTSD, where the traumatic event is persistently re-experienced in various distressing and unwanted ways. These are not merely fleeting memories; they are intense, involuntary intrusions that can feel as real and overwhelming as the original event itself. They disrupt a person’s present moment, making it incredibly difficult to escape the shadow of the past trauma.
These distressing re-experiences manifest in several specific ways:

Avoidance symptoms represent the individual’s persistent and often desperate efforts to steer clear of anything associated with the trauma. This is a powerful, albeit unhelpful, coping mechanism aimed at reducing the intense distress caused by intrusive thoughts, memories, or external reminders. However, this avoidance often leads to significant limitations in daily life, restricting activities, narrowing one’s world, and ultimately isolating the individual.
These avoidance behaviors manifest in specific patterns:

This category encompasses a wide range of negative shifts in how a person thinks about themselves, others, and the world, as well as significant changes in their emotional state. These symptoms often develop or worsen after the trauma and can profoundly impact relationships, self-perception, and general outlook on life, sometimes making it difficult to find joy or connection.
These cognitive and mood symptoms include:

This category describes persistent symptoms of increased arousal and reactivity, indicating that the individual’s “fight or flight” system remains chronically hyperactive. These symptoms often lead to significant distress and impairment, making it incredibly difficult to relax, concentrate, or feel safe in everyday situations, contributing to a constant sense of being on edge.
These arousal and reactivity symptoms include:
For a formal diagnosis of PTSD, these numerous and often debilitating symptoms must be present for more than one month and cause significant distress or impairment in social, occupational, or other important areas of functioning. It’s important to note that if similar symptoms are present for less than a month, it might be classified as Acute Stress Disorder; however, careful monitoring is crucial as Acute Stress Disorder can often evolve into PTSD.
When these 17 symptoms combine and persist, they can profoundly impact an individual’s quality of life. They interfere with maintaining healthy relationships, performing effectively at work or school, engaging in self-care, and finding joy in activities once enjoyed. Recognizing this comprehensive list of symptoms is the vital first step towards understanding the severity of the condition and, most importantly, seeking appropriate help. With the right support and PTSD treatment, individuals can begin their journey towards recovery and healing from the effects of trauma.

In conclusion, understanding the 17 PTSD symptoms is crucial for identifying when professional help is needed. At Mind Above Matter, we are dedicated to providing comprehensive and compassionate mental health services. We specialize in various levels of care, including outpatient therapy and more intensive programs, to help individuals navigate the complexities of trauma and its impact.
Our clinics in Keller and Burleson, Texas, offer a supportive environment for healing. Additionally, for all Texas residents, we provide convenient virtual outpatient therapy options, ensuring access to care no matter where you are in the state. For those experiencing deeper, more pervasive impacts of trauma, our complex trauma treatment approaches are designed to address the unique challenges of enduring psychological injury.
You can learn more about our specialized trauma care and services. Don’t hesitate to take the first step towards healing and reclaiming your well-being. If you or someone you know is struggling with the persistent effects of trauma, remember that you are not alone, and effective PTSD treatment is available.
1. what are the 17 symptoms of PTSD?
The 17 symptoms of PTSD include flashbacks, nightmares, emotional numbness, irritability, difficulty sleeping, avoidance of reminders, negative mood, memory problems, difficulty trusting others, feelings of hopelessness, and self-destructive behavior.
2. How is PTSD diagnosed?
PTSD is diagnosed through a clinical evaluation, including a detailed history of traumatic events and symptoms. A mental health professional will assess how symptoms affect daily functioning.
3. Can PTSD symptoms appear immediately after trauma?
PTSD symptoms can appear immediately after a traumatic event, but it’s common for symptoms to develop within the first three months or even years later.
4. Can PTSD symptoms improve over time?
With proper treatment, PTSD symptoms can improve. Therapy, such as cognitive behavioral therapy (CBT), and medication can help manage symptoms and improve quality of life.
5. How long can PTSD last?
PTSD can last for months or years, but with treatment, many individuals experience a reduction in symptoms and find healthier ways to cope. Early intervention is key to recovery.
These FAQs provide additional clarity on PTSD, answering common questions
Related: What are the 5 Levels of Trauma Care?
Summer often brings thoughts of long, carefree days, vacations, and outdoor fun. While it can be a season of joy and relaxation, the warmer months can also present unique challenges to our mental well-being. From shifts in routine to potential social pressures or even seasonal affective patterns as a result of seasonal depression, it’s important to be proactive about your mental health.
At Mind Above Matter, we’re committed to supporting your holistic well-being year-round, and that includes providing valuable summer mental health tips to help you thrive.

The sun’s warmth and light can be a mood booster, but it’s important to engage with summer mindfully.

While school’s out and vacations are common, summer can paradoxically lead to increased feelings of isolation for some, especially children and adolescents removed from their regular social structures.

Summer’s relaxed vibe can disrupt healthy routines, which are often cornerstones of good mental health. Balance flexibility with a gentle structure.

Effective summer mental health tips always include a focus on intentional self-care and robust coping strategies.
While these summer mental health tips can be incredibly helpful, it’s vital to recognize when professional support is needed. If feelings of anxiety, depression, or isolation become overwhelming, persistent, or interfere with your daily life, please know that reaching out is a sign of immense strength.

Summer offers wonderful opportunities for joy and renewal, but it also brings unique considerations for our mental well-being. By proactively implementing these summer mental health tips, you can navigate the season with greater peace, connection, and resilience.
If you or a loved one needs support this summer, please don’t hesitate to reach out. Mind Above Matter is dedicated to providing comprehensive and compassionate mental health services. We have convenient clinics in Keller and Burleson, Texas, and also offer flexible virtual therapy options for all Texas residents. Contact us today to schedule a free assessment and take the first step toward a healthier, happier summer.
Related: Why Summer Break is Essential for Students’ Mental Health
Mind Above Matter Donates to United Texas Flood Relief, Commits to Supporting Community Recovery
KELLER, TEXAS – July 18, 2025 – Mind Above Matter, a leading mental health clinic serving Texas, announced a significant donation to United Texas Flood Relief, committing support to communities devastated by the recent severe flooding across the state. This contribution aims to assist with immediate needs and foster long-term rebuilding efforts, acknowledging the profound mental health impact of such widespread disasters.
The recent widespread flooding in Texas has caused immense physical damage and, equally important, has placed a significant emotional and psychological burden on countless individuals and families. Mind Above Matter recognizes the profound impact such events have on mental well-being and the critical need for comprehensive community support during recovery. As mental health advocates, we understand that healing extends beyond physical reconstruction to encompass emotional resilience.
In response to these challenges, Mind Above Matter has contributed to United Texas Flood Relief. This organization was chosen for its proven dedication to providing both immediate aid and fostering long-term recovery, directly aligning with Mind Above Matter’s commitment to rebuilding lives and promoting resilience within our Texas communities. Their on-the-ground efforts are vital in helping those most affected navigate the aftermath.
“Our hearts go out to everyone affected by the recent floods,” said Yossi Tress, CEO of Mind Above Matter. “Beyond the physical devastation, we understand the immense emotional toll these events take. Supporting United Texas Flood Relief is a direct extension of our mission to foster healing and resilience within our communities as they navigate this challenging recovery. We stand in solidarity with all Texans.”
About Mind Above Matter: Mind Above Matter is a leading mental health clinic dedicated to providing compassionate, evidence-based care to individuals and families across Texas. With convenient locations in Keller and Burleson, and virtual therapy available statewide, Mind Above Matter offers a comprehensive range of services, including Partial Hospitalization Programs (PHP), Intensive Outpatient Programs (IOP), and individual therapy, all designed to foster healing and promote lasting well-being.
About United Texas Flood Relief: United Texas Flood Relief is a non-profit organization dedicated to providing immediate relief and fostering long-term recovery for Texas communities impacted by severe flooding. Through direct aid, community support, and strategic partnerships, the organization works tirelessly to help Texans rebuild their homes, their lives, and their communities.
Support Texas Recovery: You can also contribute to the ongoing relief efforts. Donate to United Texas Flood Relief here.
Anxiety, a natural human emotion, can sometimes escalate into intense fears that profoundly disrupt daily life. Among the many forms anxiety can take, two distinct conditions, agoraphobia and social phobia (also known as social anxiety disorder), are frequently confused or experienced concurrently. While both involve significant anxiety and subsequent avoidance behaviors, their core fears are fundamentally different. Agoraphobia primarily centers on a pervasive fear of places or situations from which escape might be difficult, or where immediate help might not be available if distressing symptoms arise, often leading to a reluctance to enter public spaces.
In contrast, social phobia is characterized by an overwhelming and persistent fear of social situations where an individual might be subjected to scrutiny, judgment, or potential humiliation by others. The fear in social phobia is not inherently about the physical location itself, but rather the social interaction that takes place within that environment. Understanding these distinctions is paramount for accurate self-assessment and for developing targeted, effective strategies to manage these challenging and often debilitating fears.
Agoraphobia is classified as an anxiety disorder, marked by an intense and often irrational fear of specific situations or places. These can include open spaces like parking lots, enclosed spaces such as elevators or crowded stores, public transportation, standing in long lines, being immersed in a large crowd, or even the simple act of being outside of one’s home alone. The underlying fear is typically less about the place itself and more about the potential for experiencing incapacitating panic-like symptoms or other embarrassing physical reactions in that setting, coupled with the perceived inability to escape or receive timely assistance. This fear can be so overwhelming that it dictates daily decisions, significantly narrowing one’s world.
As a direct consequence of this profound fear, individuals with agoraphobia frequently engage in extensive avoidance behaviors. They may go to great lengths to bypass feared situations, sometimes relying heavily on others to perform errands or attend events on their behalf. In its most severe manifestations, this avoidance can lead to an individual becoming entirely housebound, as their home transforms into the sole perceived safe haven. The mere anticipation of entering a feared situation can trigger intense anxiety, creating a self-perpetuating cycle where avoidance reinforces the erroneous belief that these places are inherently dangerous, rather than manageable with coping strategies.
Social phobia, officially known as social anxiety disorder, is characterized by an intense and persistent fear of social or performance situations where an individual fears being exposed to the scrutiny of others. This fear is often rooted in the apprehension of acting in a way that will be humiliating, embarrassing, or lead to negative judgment. It’s crucial to differentiate this from mere shyness; social phobia is a debilitating anxiety that can profoundly disrupt an individual’s daily life, academic pursuits, professional career, and personal relationships. Common feared situations are diverse and can include public speaking, eating or drinking in public, initiating or maintaining conversations, attending social gatherings or parties, meeting new people, or even simply being observed while performing a routine task.
The central and most pervasive component of social phobia is the overwhelming concern about how others will evaluate them. Individuals might worry excessively about visible signs of anxiety, such as blushing, sweating, trembling, or stuttering, believing these physical manifestations will lead to ridicule or rejection. They may also obsess over saying the “wrong thing” or appearing awkward. This pervasive fear frequently culminates in extensive avoidance of social situations altogether, or enduring them with immense discomfort and a range of physical symptoms, including a racing heart, shortness of breath, dizziness, or nausea. The constant internal battle against these fears can be exhausting and isolating.
While agoraphobia and social phobia are recognized as distinct anxiety disorders, it is quite common for them to coexist or influence each other in complex ways. An individual who initially struggles with severe, unexpected panic attacks might, over time, develop agoraphobia as they begin to fear situations where a panic attack could potentially occur, including various social settings. This leads to a generalized fear of being in public or away from a “safe” person or place.
Conversely, someone experiencing intense social phobia might progressively restrict their social activities to such an extreme extent that their world dramatically narrows. This severe avoidance of social events can eventually lead them to fear leaving their home or other perceived safe spaces, thereby developing secondary agoraphobic tendencies. The shared and most significant element connecting these two conditions is the pervasive pattern of avoidance, which ultimately leads to a constriction of one’s life, limiting opportunities for personal growth, meaningful employment, and vital social connection. Accurately discerning whether one’s primary fear is rooted in the fear of situations without easy escape (agoraphobia) or the fear of negative social judgment (social phobia), or a complex combination of both, is a critical step in developing an effective social phobia treatment plan aimed at regaining freedom and confidence.
Both agoraphobia and social phobia, left unaddressed, can exert profound and far-reaching negative impacts on an individual’s daily life and overall well-being. The pervasive avoidance behaviors characteristic of these conditions often lead to severe social isolation, significantly limiting opportunities for forming and maintaining friendships, romantic relationships, and engaging in community activities. Career progression can also be severely hindered, as many professional roles and opportunities for advancement inherently require public speaking, networking, collaborative teamwork, or leadership, all of which individuals with these phobias might find overwhelmingly challenging to perform.
Beyond the immediate social and professional spheres, the constant anticipation and lived experience of intense anxiety can take a significant toll on both mental and physical health. The chronic stress associated with these conditions can contribute to feelings of hopelessness, exacerbate symptoms of depression, and even worsen other physical health conditions. The reduced freedom and diminished ability to engage spontaneously with the world can dramatically decrease one’s overall quality of life, transforming even seemingly simple errands or casual social calls into insurmountable and terrifying challenges.
Effectively managing agoraphobia and social phobia typically involves a comprehensive, multi-faceted approach, often guided by mental health professionals. Exposure therapy, a core and highly effective component of Cognitive Behavioral Therapy (CBT), is central to treatment. This involves gradually and systematically exposing oneself to feared situations or places, starting with scenarios that provoke minimal anxiety and progressively increasing the challenge. This structured process helps individuals learn that their feared outcomes rarely materialize and that their anxiety response can diminish significantly over time through repeated, safe encounters. Alongside exposure, incorporating relaxation techniques such as deep breathing exercises, progressive muscle relaxation, and mindfulness practices are crucial tools that can be employed in the moment to reduce acute physical anxiety symptoms.
Beyond these in-the-moment strategies, psychoeducation plays a vital role in empowering individuals to understand the underlying nature of anxiety and to actively challenge distorted or catastrophic thought patterns. Learning to identify and reframe negative thoughts (e.g., “everyone will stare at me,” “I’ll make a fool of myself,” “I’ll be trapped and can’t get out”) is central to managing both conditions. Building a strong and supportive network, whether through trusted friends and family, or by participating in specialized support groups, can provide invaluable validation, encouragement, and a sense of shared experience on the journey towards overcoming these fears. For those seeking structured and intensive support, outpatient therapy programs can provide a robust social phobia treatment plan, offering comprehensive therapeutic interventions without requiring an inpatient stay, allowing individuals to integrate healing into their daily lives.
Understanding the distinctions and overlaps between agoraphobia and social phobia is the first step, but taking action is where true healing begins. At Mind Above Matter, we are dedicated to providing compassionate, evidence-based care to help you or your loved one navigate these intense fears, build resilience, and reclaim a life of greater freedom and confidence.
If you are struggling with agoraphobia, social phobia, or any other mental health challenge, we invite you to reach out. We offer comprehensive mental health services designed to support your unique needs, including group therapy, medication management, and specialized programs. Contact Mind Above Matter today to learn more about our approaches and schedule a free assessment. Our clinics are conveniently located in Keller and Burleson, Texas, and we also offer virtual therapy services for all Texas residents. Your journey to well-being matters to us.
Related: Understanding DSM-5 Social Phobia (Social Anxiety Disorder): A Diagnostic Perspective
Social phobia, officially recognized in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) as Social Anxiety Disorder, is a condition that extends far beyond mere shyness or occasional discomfort in social settings. It is a deeply impactful mental health condition characterized by an intense, persistent fear of social situations where an individual anticipates being scrutinized, judged, or humiliated by others. This pervasive fear can be so profound that it leads to significant emotional distress and considerable impairment across various crucial areas of life, including academic, professional, and personal spheres.
The DSM-5 serves as the authoritative guide used by mental health professionals to diagnose a wide range of mental disorders. It provides a standardized and rigorous set of criteria that must be met for a diagnosis of Social Anxiety Disorder, ensuring consistency and accuracy in clinical assessment across different practitioners and settings. For individuals experiencing these challenging symptoms, understanding these diagnostic benchmarks is crucial for recognizing their struggles as a treatable condition. For clinicians, a clear and precise diagnosis forms the indispensable foundation for developing and implementing an effective and tailored social phobia treatment plan.
The DSM-5 meticulously outlines specific criteria that must be present for a diagnosis of Social Anxiety Disorder to be made. The primary and most central criterion is a marked fear or intense anxiety about one or more social situations where the individual anticipates being exposed to possible scrutiny by others. This can encompass a broad spectrum of scenarios, such as engaging in social interactions like having a conversation or meeting unfamiliar people, being observed while performing routine activities like eating or drinking, or performing in front of an audience, such as giving a speech or presentation. The underlying fear is that they will act in a way, or display anxiety symptoms (like blushing, sweating, or trembling), that will be negatively evaluated, leading to humiliation, embarrassment, or rejection.
Furthermore, these feared social situations almost invariably provoke immediate fear or anxiety in the individual. Consequently, these situations are either actively avoided altogether, or if they must be endured, they are done so with intense fear or anxiety, causing significant distress. A critical aspect of the diagnosis is that the fear or anxiety experienced must be disproportionate to the actual threat posed by the social situation and also to the sociocultural context in which it occurs. For a formal diagnosis of DSM-5 social phobia to be established, this fear, anxiety, or avoidance must be persistent, typically lasting for a minimum of 6 months or more, and must cause clinically significant distress or impairment in social, occupational, or other important areas of functioning. It’s also essential that the disturbance is not attributable to the physiological effects of a substance (e.g., a drug of abuse, medication) or another underlying medical condition, nor is it better explained by another mental disorder.
The DSM-5 offers a specific qualifier for Social Anxiety Disorder to help clinicians further refine the diagnosis: the “Performance only” specifier. This specifier is applied if the individual’s fear is strictly limited to speaking or performing in public situations. This means that individuals with this particular specifier typically do not experience significant anxiety in other common social interactions, such as engaging in casual conversations, meeting new acquaintances, or participating in small group discussions. This distinction is valuable as it helps to narrow the focus of the anxiety and can sometimes lead to a more targeted approach in social phobia treatment.
Beyond these core diagnostic criteria, individuals diagnosed with Social Anxiety Disorder often exhibit a range of associated features that can complement the clinical picture. These may include behavioral patterns such as being excessively submissive in social interactions, adopting a rigid body posture, avoiding direct eye contact, or speaking with an unusually soft or hesitant voice. Cognitively, they may be overly self-critical, constantly monitoring their own behavior, and hold negative beliefs about their social abilities. They might also experience difficulty being assertive or demonstrate impaired social skills, not due to a lack of understanding, but due to anxiety-driven avoidance of practice. Physically, common anxiety responses in feared social situations include noticeable blushing, excessive sweating, trembling, a racing heart, shortness of breath, or gastrointestinal distress.
When a mental health professional is evaluating an individual for Social Anxiety Disorder, a crucial step involves a process known as differential diagnosis. This means carefully distinguishing DSM-5 social phobia from other conditions that might present with similar symptoms but have different underlying causes or diagnostic criteria. For instance, it is vital to differentiate it from normal shyness, which, while involving some discomfort, does not typically lead to the same level of pervasive distress or significant functional impairment in daily life. Social Anxiety Disorder also differs from Panic Disorder, where the primary fear is centered on having an unexpected panic attack, whereas in social anxiety, the fear is specifically about negative evaluation or embarrassment within a social context. Generalized Anxiety Disorder (GAD), which involves broad, persistent, and excessive worry about multiple life domains, also needs to be considered, as its focus is not limited to social situations.
Furthermore, Social Anxiety Disorder frequently co-occurs with other mental health conditions, a phenomenon known as comorbidity. This means that an individual may experience Social Anxiety Disorder alongside one or more other diagnosable conditions. Common co-occurring disorders include other anxiety disorders (such as Generalized Anxiety Disorder or Panic Disorder), Major Depressive Disorder, and Substance Use Disorders, which individuals may develop as a maladaptive coping mechanism for their anxiety. The presence of comorbid conditions can significantly complicate both the diagnostic process and the subsequent social phobia treatment plan, necessitating a comprehensive and holistic assessment to ensure all contributing factors to an individual’s distress are identified and addressed effectively.
The pervasive fear and avoidance behaviors intricately linked with Social Anxiety Disorder can exert a profound and debilitating impact on nearly every facet of an individual’s daily functioning and overall quality of life. Academically, students grappling with this condition may find themselves struggling immensely with tasks such as delivering presentations, participating in group projects, or even simply asking questions in class, which can directly affect their learning outcomes and academic performance. Professionally, the condition can severely limit career advancement opportunities; individuals might avoid job interviews, decline promotions that inherently require public speaking or leadership roles, or find it exceptionally challenging to network and build professional relationships, thus hindering their professional growth and potential.
Socially, the consequences of DSM-5 social phobia can lead to significant and painful isolation. Individuals may actively avoid parties, dating, or even casual interactions with friends and family, leading to profound feelings of loneliness, alienation, and a diminished sense of belonging within their communities. Beyond the social and professional spheres, the constant anticipation and lived experience of intense anxiety can take a tremendous toll on both mental and physical health. This chronic stress can contribute to feelings of hopelessness, exacerbate symptoms of depression, and even lead to or worsen other physical health conditions. The reduced freedom and ability to engage spontaneously with the world can dramatically diminish one’s quality of life, transforming even seemingly simple errands or social calls into insurmountable and terrifying challenges.
A formal diagnosis of Social Anxiety Disorder, meticulously based on the DSM-5 criteria, represents a critical and foundational step in guiding an effective social phobia treatment journey. Without a clear and accurate understanding of the specific condition an individual is facing, therapeutic interventions may be misdirected, less efficient, or even ineffective. A precise diagnosis empowers mental health professionals to select and implement evidence-based therapies that are specifically designed to address the core fears, cognitive distortions, and avoidance behaviors uniquely associated with social anxiety. This targeted approach ensures that treatment efforts are optimized for the best possible outcomes.
Once a diagnosis is established, individuals can access tailored interventions such as Cognitive Behavioral Therapy (CBT), which is widely recognized as highly effective in helping people identify and challenge negative thought patterns that fuel their anxiety. CBT also involves gradual, systematic exposure to feared social situations in a controlled and supportive manner, helping individuals to slowly desensitize themselves to their triggers and build confidence. A formal diagnosis also plays a crucial role in validating an individual’s struggles; it helps them understand that their challenges are part of a recognized and treatable medical condition, thereby reducing feelings of shame, self-blame, or isolation, and empowering them to engage more fully and hopefully in their recovery journey.
Understanding the diagnostic criteria for DSM-5 social phobia is a vital first step, but true healing comes from taking action. At Mind Above Matter, we are dedicated to providing compassionate, evidence-based care to help individuals navigate the complexities of social phobia, build resilience, and reclaim a life of greater freedom and confidence. Our team of experienced professionals understands the unique challenges posed by social phobia and is equipped to develop personalized social phobia treatment plans.
If you or someone you know is struggling with the pervasive fears associated with social phobia, we invite you to reach out. We offer comprehensive mental health services designed to support your unique needs, including group therapy, medication management, and specialized programs tailored to foster growth and well-being. Contact Mind Above Matter today to learn more about our approaches and schedule a free assessment. Your journey to a calmer, more connected life starts here.
Related: Understanding Agoraphobia and Social Phobia
Navigating mental health challenges can often feel isolating. While individual therapy offers invaluable one-on-one support, there’s a unique and profound strength found in shared experiences. Group therapy, where a small group of individuals meets regularly with one or more therapists to address common issues, provides a powerful avenue for healing and growth.
At Mind Above Matter, we understand the transformative impact of collective support. This guide will explain the realistic benefits of group therapy for mental health and well-being.
The unique dynamics of a group setting offer distinct advantages that complement individual therapeutic work:

While group therapy isn’t a one-size-fits-all solution, it is highly effective for a wide range of concerns. Individuals dealing with depression, anxiety (including social anxiety), substance use recovery, grief, trauma, social isolation, and relationship issues often find immense value. It can also serve as an excellent complement to individual therapy, providing a different dimension of support and learning.
At Mind Above Matter, we believe in the profound healing power of connection and community. That’s why we strategically integrate group therapy into all of our treatment programs. Our approach emphasizes evidence-based practices, delivered in compassionate and inclusive environments.
Our expert clinicians skillfully lead groups, ensuring a safe space for vulnerability, growth, and the development of practical coping skills. Whether in our PHP (Partial Hospitalization Program) or IOP (Intensive Outpatient Program), group therapy is a core component designed to foster resilience and lasting well-being.

The benefits of group therapy extend far beyond the session room, offering a powerful pathway to healing, personal growth, and lasting connection. By sharing experiences, gaining diverse insights, and practicing new skills in a supportive community, individuals can find strength they never knew they had.
Ready to experience the power of connection and healing? Contact Mind Above Matter today to learn more about our group therapy programs and schedule a free assessment.
Proudly serving Keller, Burleson, Irving, Waxahachie, Carrollton Farmer’s Branch, and Frisco, Texas. We also provide virtual therapy for all Texas residents.
Related: Exploring the Power of Music Therapy for Mental Wellness
If you or someone you know is struggling with addiction in Keller, TX, a Partial Hospitalization Program (PHP) could be the key to effective treatment. With the rise in addiction cases across the country, it’s essential to have specialized programs in Keller that provide comprehensive care to help people recover and rebuild their lives.
A Partial Hospitalization Program in Keller offers a structured and intensive treatment option for individuals with mental health conditions or addiction struggles. Unlike traditional outpatient care, PHP provides more support while still allowing clients to live at home. For those facing addiction, this is a crucial aspect, as it offers a balance of therapeutic care and personal space for healing.
In Keller, individuals participating in a PHP are guided through a range of therapies, including individual, group, and family counseling. These services help address the root causes of addiction, while also teaching clients essential coping skills and strategies to manage triggers and stressors in real-life scenarios. Moreover, PHPs allow for close monitoring of progress while offering a safe and familiar environment for recovery.
Take, for instance, the story of Jenna, a resident of Keller who was battling a severe alcohol addiction. By enrolling in a Partial Hospitalization Program, Jenna received personalized therapy tailored to her needs. The structure of the program helped her stay committed to her treatment plan while still maintaining a connection to her family and friends. Over time, Jenna was able to regain control of her life, using the tools she learned in the PHP to stay sober and healthy.
PHPs are designed to address a range of mental health issues, including but not limited to:
By focusing on these conditions through structured treatment and therapy, Partial Hospitalization Programs Keller provide a well-rounded approach to mental health and addiction care.

Yes, Keller Partial Hospitalization Programs offers several programs specializing in addiction treatment. These programs provide the necessary medical supervision, therapy, and support that individuals need to recover from substance abuse.
One of the key advantages of PHPs in Keller is the flexibility they offer. These programs are designed to fit around a person’s life, allowing them to engage in therapy while still managing daily responsibilities. For individuals like Mark, a local resident of Keller, the ability to receive care without leaving home made a huge difference in his recovery. Mark was able to attend his sessions and participate in group therapy, all while feeling connected to his community and family.
Moreover, PHPs that specialize in addiction treatment in Keller often incorporate various therapeutic modalities, including cognitive-behavioral therapy (CBT), dialectical behavior therapy (DBT), and holistic treatments like yoga or mindfulness. These therapies help clients work through emotional and psychological barriers to their addiction, while also providing life skills training to prevent relapse.
If you’re considering treatment for addiction, it’s important to find a program that offers personalized care tailored to your needs. The Keller Partial Hospitalization Program is designed to help people heal in ways that work for them, offering a supportive environment for lasting recovery.
At Mind Above Matter, we specialize in compassionate, client-focused mental health services. Our team is dedicated to offering personalized care in safe, familiar environments, whether in a school, home, or long-term care setting. We believe in reducing barriers to treatment and offering the flexibility needed to support lasting healing. Contact us today to start your journey toward a healthier mind and a brighter future.
Contact us today to learn more about the Partial Hospitalization Programs available in Keller and how they can help you or your loved one heal.
1. What is the difference between Partial Hospitalization and inpatient care?
Inpatient care requires a person to stay at the facility 24/7, while Partial Hospitalization Programs allow individuals to receive intensive treatment during the day and return home in the evening. This flexibility makes PHPs a great option for those who need support but want to maintain some level of independence.
2. How long does a Partial Hospitalization Program typically last?
The duration of a PHP can vary depending on the individual’s needs. Typically, programs last anywhere from a few weeks to several months, with some individuals needing extended care.
3. Will insurance cover a Partial Hospitalization Program?
Many health insurance plans provide coverage for Partial Hospitalization Programs, especially for those being treated for addiction or mental health disorders. It’s best to check with your insurance provider to understand the specifics of your coverage.
4. What can I expect during a typical day in a Partial Hospitalization Program?
Each day in a PHP typically includes therapy sessions, group activities, skill-building workshops, and time for individual reflection. You’ll work closely with a team of therapists, counselors, and medical staff to create a personalized treatment plan for recovery.
If you're considering an Intensive Outpatient Program (IOP) for addiction or mental health issues in Keller, it's natural to have many questions. The Outpatient Program provides structured treatment while allowing you to continue your daily responsibilities, such as work or school. But is it the right fit for you? Let’s explore how to determine if an IOP is the ideal treatment option for you in Keller, TX.
An Intensive Outpatient Program at Keller can be a game-changer if you're facing challenges with addiction or mental health. But how do you know if it’s the right path for you? Here are a few key indicators:
Take the example of Sarah, a Keller resident who was struggling with anxiety and depression but wanted to continue her full-time job as a marketing professional. After consulting with a mental health professional, Sarah was referred to an IOP. It was the perfect fit, offering her therapy sessions in the evenings and allowing her to receive the support she needed while continuing with her life.
If you feel like you have a mild to moderate condition and you’re ready to commit to a structured program, an IOP may be right for you. However, it’s essential to consult with a healthcare professional who can evaluate your unique situation and guide you through the decision-making process.
Yes! One of the biggest benefits of an Intensive Outpatient Programs Keller is the ability to maintain your regular routine. In Keller, you can attend therapy sessions at times that fit your schedule, whether evenings or weekends, without taking time off from work or school.
This flexibility makes IOP a highly effective option for individuals who want to continue with their daily activities while receiving professional help. For example, many IOP centers offer flexible scheduling, such as evening or weekend therapy sessions, so you can still meet your commitments.
In fact, many clients find that keeping a routine, including work or school, is part of their healing process. Engaging in regular activities, maintaining social connections, and focusing on day-to-day tasks help them build a sense of normalcy while also making progress in their recovery.
Keller Intensive Outpatient Programs are designed to treat a variety of addiction and mental health issues, including but not limited to:
For instance, John, a local resident of Keller, struggled with anxiety and alcohol dependency. He was able to balance his full-time job with a Keller Intensive Outpatient Program that treated both his mental health and addiction issues. Through a combination of individual therapy and group support, he found a path toward recovery while staying on track with his professional goals.

An IOP is structured yet flexible, with several key elements that make it an effective treatment choice:
Mind Above Matter is a compassionate, client-focused mental health care provider based in Keller, TX. Our mission is to support individuals through personalized treatment in comfortable, safe environments. Whether you're seeking help with anxiety, depression, addiction, or any other mental health issue, we are here to guide you through your healing journey.
Ready to take the next step? Contact us today to schedule an evaluation and explore how our Intensive Outpatient Programs can support you on your path to recovery.
People Also Ask
Yes! One of the main advantages of IOPs is their flexibility. Many programs in Keller provide evening or weekend sessions, allowing you to keep up with work or school commitments.
Inpatient treatment requires you to stay at a facility full-time, whereas outpatient treatment, like IOP, allows you to live at home and continue with your daily activities while receiving structured therapy and support.
While IOPs are excellent for mild to moderate addiction, individuals with severe addiction may benefit from inpatient treatment, where they can receive round-the-clock care.
The duration of IOPs can vary, but most programs last between 6 and 12 weeks. The intensity of the program will depend on your individual needs and progress.
FORT WORTH, TX — February 20, 2026 — Mind Above Matter, in partnership with Santé Center for Healing and a coalition of leading North Texas behavioral health providers,recently held the 2026 Resiliency & Recovery Conference of Fort Worth. This premier clinical event took place at the Lena Pope Center, bringing together licensed clinicians and interns for a comprehensive day of advanced trauma-informed training and recovery innovation.
The conference offered 6 CE hours and featured a diverse curriculum designed to address the most pressing challenges in modern behavioral health, including Opioid Use Disorder (OUD), family system dynamics, and neurobiological regulation.
Mind Above Matter Highlights Innovation in MAT
A cornerstone of this year’s program was a deep dive into Medication Assisted Recovery (MAR). Lisa Wedgeworth, Program Therapist at Mind Above Matter, presented "Benefits of Medication Assisted Recovery in Opioid Use Disorder." As OUD continues to impact communities across Texas, Wedgeworth’s session provides clinicians with essential frameworks for utilizing MAR as the gold standard for preventing overdose and stabilizing vulnerable populations, including homeless and pregnant clients.
“At Mind Above Matter, we believe in providing a 'Full-Circle' approach to care,” says Executive Director of Strategic Partnerships, Jesse Cordova. “Lisa’s presentation underscores our commitment to evidence-based practices that allow clients to resolve psychosocial stressors while maintaining physical and emotional stability.”
A Collaborative Approach to Healing
The conference featured a powerhouse lineup of industry leaders addressing a wide spectrum of recovery topics:
Commitment to Clinical Excellence
The event is supported by a robust network of 2026 sponsors, including Arise Recovery Centers, Eating Recovery Center, Well Mind Therapy Center, and Lifepoint Behavioral Health, among others. Credits are provided through the Texas Certification Board of Alcoholism and Drug Abuse Counselors and the Texas State Boards for Professional Counselors, Marriage and Family Therapists, and Social Worker Examiners.
Mind Above Matter is a premier behavioral health provider dedicated to intentional, client-centered care. Through innovative programming and community collaboration, Mind Above Matter strives to create lasting resilience for individuals and families navigating the journey of recovery.
DENTON, TX — Mind Above Matter (MAM), a leading provider of restorative behavioral health services in North Texas, is proud to announce a new partnership with Denton Independent School District. This collaboration introduces the IMatter program to the district, with a primary clinical site established at Fred Moore High School.
The IMatter program is an integrated, school-based initiative designed to meet students exactly where they are. By providing Partial Hospitalization (PHP) and Intensive Outpatient (IOP) levels of care directly within the district community. IMatter bridges the critical gap between traditional weekly therapy and inpatient hospitalization.
“Our mission is to help students navigate their emotional challenges in a familiar, reassuring environment,” said Joann Gillen, Executive Director of IMatter. “By integrating our clinical team into the Denton ISD community, we ensure that students don’t have to choose between their education and their mental health. We are bringing them one step closer to whole.”
The IMatter program at Fred Moore High School offers:
This partnership addresses a growing need for accessible adolescent mental health services in North Texas. IMatter provides students with concrete coping strategies and behavioral support to stabilize in crisis and foster long-term resilience within the classroom.
For more information about the IMatter program, please visit www.mindabovematter.com or contact heal@mabovem.com.
About Mind Above Matter
Mind Above Matter provides restorative, full-circle mental health care across North Texas. Through their specialized IMatter school partnerships and clinical facilities, they are dedicated to helping adolescents and adults move closer to whole. With a focus on clinical integrity and compassionate support, Mind Above Matter is redefining the path to mental wellness.